 
Two of the main sponsors of P4P programs are government agencies and health insurance plans. These programs reward hospitals, physician practices and other providers based on their performance and reporting of select measures. Many believe “pay-for-performance” initiatives will help providers attain the Triple Aim. Providers will be incentivized for engaging in their patients’ care, keeping them healthy, and reducing the utilization of hospitals and emergency departments. To meet this goal, physicians need more efficient and cost-effective ways to care for their patients, avoiding unnecessary tests or procedures. The final goal of the Triple Aim is lowering per capita healthcare costs, measured as a total cost per member (or citizen) per month. Providers look at six measurements: Was care safe, effective, timely, patient-centered, equitable or fair, and efficient? The second element of the Triple Aim is an improved experience of care on the patient’s part. Population health management tends to focus on high-risk patients, because they generate the majority of health costs. They can do so by supplying preventive and chronic care to all their patients, and educating their population on how to support and manage their own healthcare needs during and between visits to their facility. Population health management calls for providers to keep a patient population as healthy as possible, minimizing the need for expensive emergency department visits, hospitalizations, tests, and procedures. The Triple Aim is a framework for optimizing health system performance by focusing on 1) the health of a population, 2) the experience of care for individuals within that population, and 3) the per capita cost of providing that care. 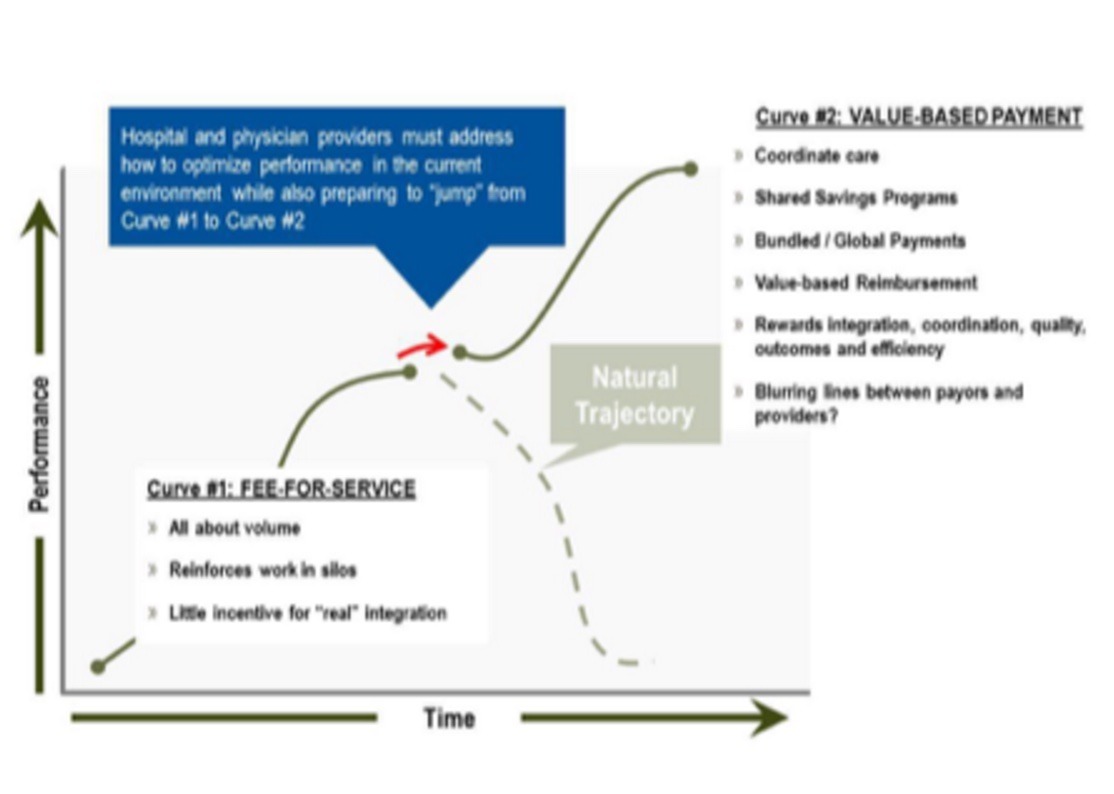
Today, the organization remains committed to improving healthcare. Founded in 1980, the IHI initially focused on healthcare best practices and reducing defects and errors in specific areas, such as the emergency department or ICU. The Triple Aim was introduced in 2007 by the Institute for Healthcare Improvement. This is part of an ongoing series designed to help readers understand the implications of reform.Īs healthcare continues to move away from fee-for-service medicine in favor of outcomes-based medicine, providers will shift their goals to align with a new initiative – the Triple Aim of Healthcare. Supplier success in a post‐reform healthcare market depends on many factors, including a fundamental and thorough understanding of the foundation of healthcare reform. 2 The Triple Aim framework, which conveys the idea that health systems need to simultaneously optimize over multiple interlinked yet diverse goals including care experience, population health, and per-capita costs, 3 may provide a model for incorporating disparity reduction into the goals of payment reform.Pay-for-performance programs are intended to improve population health and the patient experience, while reducing cost Hence, large-scale national reform to mitigate these marked disparities is needed. 1 These disparities have persisted for decades despite targeted interventions that have been implemented locally to address the patient-, clinician-, and system-level causes. According to data from 2009 to 2017, joint replacements were less common for Black Medicare beneficiaries compared with White beneficiaries (in 2017, rates of 2.80 total hip replacements and 6.13 total knee replacements both per 1000 beneficiaries for Black beneficiaries and 4.77 total hip replacements and 9.93 total knee replacements both per 1000 beneficiaries for White beneficiaries), and income was a significant moderator of this relationship. Because of the clinical benefits of these procedures, racial and ethnic– and income-based disparities in the use and outcomes of these surgical procedures are particularly troubling. 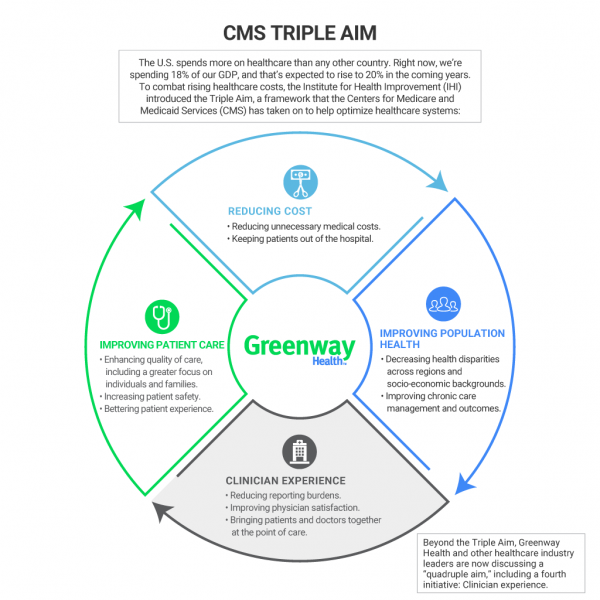
Elective total hip and knee replacements (“joint replacements”) are effective treatments for end-stage osteoarthritis.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
